Endodontics Clinic
Services
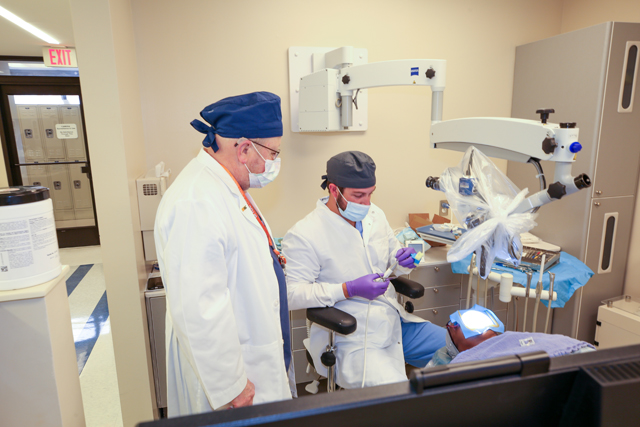
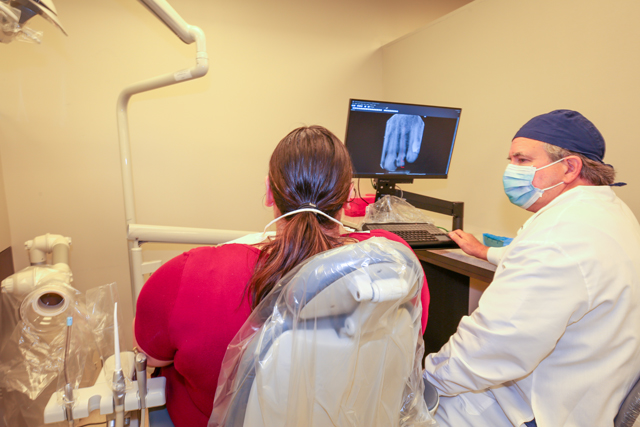
Treatment provided in the Advanced Endodontics Clinic at the UTHSC College of Dentistry covers the full scope of contemporary endodontic dental care. Using the latest technologies in dental microscopy, 3D imaging techniques, diagnostic methods and advanced surgical and restorative techniques, treatment offered in the Advanced Endodontics Clinic reflects current best practices. Some of the many services our residents and faculty members provide for their patients include:
- Non-surgical endodontics (a "root canal")
- Non-surgical retreatment
- Post cementation
- Core-build ups with composite or amalgam alloy
- Surgical endodontics (apicoectomy, root-end resection, root-end fill)
- Perforation repair
- Instrument and post retrieval
- MTA pulpotomy
- MTA apical plugs for open-apex mature teeth
- 3D Cone-beam CT imaging
- Advanced diagnosis of pain
We work closely with our colleagues from different dental disciplines (Oral Surgery, Periodontics, Prosthodontics, Orthodontics, Pediatric Dentistry, Dental Radiology, and Oral Pathology) to provide optimal comprehensive treatment for patients with challenging dental conditions and problems.
Scheduling an Appointment
The Advanced Endodontics Clinic is a limited provider; you MUST be a patient at the College of Dentistry in order to have a root canal.
You are expected to bring full payment at the first visit. The Advanced Endodontics Clinic offers treatment at deeply discounted rates and no further deductions will be offered.
Upon completion of the root canal you will be returned to your referring dentist who will complete any further treatment, such as place a crown on the tooth. We recommend you have a crown placed on any posterior tooth as soon as possible and no longer than 3 weeks following the root canal.
All teeth will receive a filling or core build-up (foundation) unless specified otherwise by your referring dentist.
Discomfort following a root canal can be managed with over the counter ibuprofen (e.g. Advil) (800 mg) 3 times a day for 2 to 3 days following treatment. Ask your resident about alternatives should you not be able to take ibuprofen. We do not routinely prescribe antibiotics.
Why choose an Endodontist?
Endodontists are dentists with at least two or three additional years of advanced specialty education in diagnosis and root canal treatment.
Because they limit their practices to endodontics, they treat these types of problems every day. They use their special training and experience in treating difficult cases, such as teeth with narrow or blocked canals, or unusual anatomy.
Endodontists may use advanced technology, such as operating microscopes, ultrasonics and digital imaging, to perform these special services.
The training, tools and techniques of endodontists have advanced a lot in recent years. Today, getting root canal treatment is often no more uncomfortable than having a filling.
Endodontists are specialists in saving teeth. Nothing can replace the natural tooth and it is our goal to maintain the oral cavity in its natural form, returning it to clinical function allowing you to smile and enjoy eating without fear from infection or pain.
Endodontic residents are dentists committed to advancing their education by enrolling in dedicated training solely in the specialty of Endodontics for two or three years.
Frequently Asked Questions
 Endodontics is the advanced specialty involved with treating and preservation of the
pulp of a tooth and its surrounding tissues. “Endo” is the Greek word for “inside”
and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth.
Root canal treatment is one type of endodontic treatment
Endodontics is the advanced specialty involved with treating and preservation of the
pulp of a tooth and its surrounding tissues. “Endo” is the Greek word for “inside”
and “odont” is Greek for “tooth.” Endodontic treatment treats the inside of the tooth.
Root canal treatment is one type of endodontic treatment
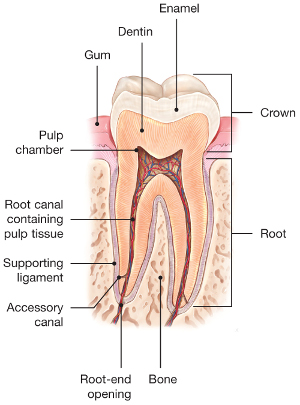
To understand endodontic treatment, it helps to know something about the anatomy of the tooth. Inside the tooth, under the white enamel and a hard layer called the dentin, is a soft tissue called the pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the surrounding hard tissues of the tooth during development.
The pulp extends from the crown of the tooth to the tip of the roots where it connects to the tissues surrounding the root. The pulp is important during a tooth’s growth and development. However, once a tooth is fully mature it can survive without the pulp, because the tooth continues to be nourished by the tissues surrounding it.
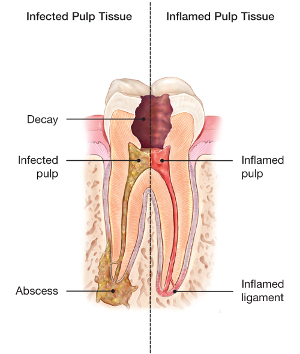 Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal,
becomes inflamed or infected. The inflammation or infection can have a variety of
causes, such as repeated dental procedures on the tooth, a crack or chip in the tooth,
but it is usually the result of deep tooth decay (cavity). In addition, trauma, an
injury to a tooth may cause pulp damage even if the tooth has no visible chips or
cracks. If pulp inflammation or infection is left untreated, it can cause pain or
lead to an abscess. When the pulp can no longer repair itself, the only two options
are extract the tooth, or save the tooth through having root canal treatment.
Endodontic treatment is necessary when the pulp, the soft tissue inside the root canal,
becomes inflamed or infected. The inflammation or infection can have a variety of
causes, such as repeated dental procedures on the tooth, a crack or chip in the tooth,
but it is usually the result of deep tooth decay (cavity). In addition, trauma, an
injury to a tooth may cause pulp damage even if the tooth has no visible chips or
cracks. If pulp inflammation or infection is left untreated, it can cause pain or
lead to an abscess. When the pulp can no longer repair itself, the only two options
are extract the tooth, or save the tooth through having root canal treatment.
A common misconception that root canals cause pain is outdated. By performing root canal treatment, you will have almost immediate pain relief. With anesthetics and advanced techniques, your comfort is greatly improved and not at all how people expect.
What are typical symptoms of root canal infection?
Depending on the cause, symptoms can be numerous and varied, including:
- Sharp, acute and intense pain, which is difficult to pinpoint
- Sharp pain when biting down on your tooth or on food
- Lingering pain after eating hot or cold foods
- Dull ache and pressure
- Tenderness (accompanied by swelling) in the nearby gums
 The treatment begins by administering a local anesthetic to relieve pain. This will
numb the tooth and surrounding area so that the treatment is no more uncomfortable
than a filling. A common misconception is that root canal treatment is a painful experience
when in actuality, it's quite the opposite.
The treatment begins by administering a local anesthetic to relieve pain. This will
numb the tooth and surrounding area so that the treatment is no more uncomfortable
than a filling. A common misconception is that root canal treatment is a painful experience
when in actuality, it's quite the opposite.
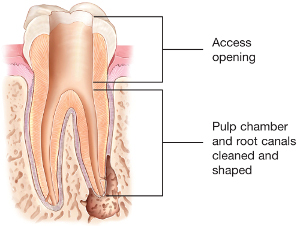
A small opening in the chewing surface of your tooth is created to gain access to the pulp. Very small instruments are used to remove dead and dying tissue and clean the pulp from the inside, allowing the root canals to be cleaned and disinfected. The canals are specially enlarged and prepared so disinfecting solutions can clean all the way throughout the root canal system and dissolve dying pulp tissue and kill any bacteria that remain.
If your tooth has a particularly bad infection, we may choose to put a disinfecting medication inside the tooth and seal it with a temporary filling and reappoint you for a second visit. This dressing kills bugs that may have persisted inside the tooth for some time and need extra time to respond to treatment.
Your resident may elect to seal your canals with a biocompatible filling material at the same appointment as it is becoming increasingly common for root canal specialists to use microscopes for these intricate and detailed procedures making the cleaning and shaping process more precise and efficient.
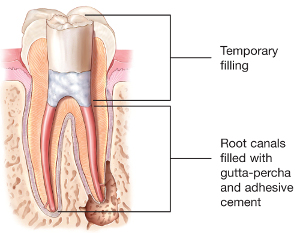 The biocompatible gutta-percha filling materials are coated with an adhesive cement
to ensure that they are completely sealed in the canals to prevent future infection.
Usually we put a permanent or temporary filling in your tooth before referring you
back to your general dentist.
The biocompatible gutta-percha filling materials are coated with an adhesive cement
to ensure that they are completely sealed in the canals to prevent future infection.
Usually we put a permanent or temporary filling in your tooth before referring you
back to your general dentist.
For a posterior tooth, generally any tooth behind the canines or “eye teeth,” your referring dentist will likely prepare the tooth for a crown, that covers the whole tooth, like a thimble, ensuring the integrity and longevity of the treatment.
For the first few days after treatment, your tooth may feel tender or sensitive, especially if there was pain or infection before the procedure. Most discomfort can be relieved by over-the-counter medication like aspirin or Advil (ibuprofen). If you have discomfort or pain that lasts more than a few days, or if there are other increasing symptoms, you must call your resident directly with the phone number on your appointment card. Prescription medications, such as antibiotics and stronger pain medications, may be indicated.
You should not chew or bite on the treated tooth until you have seen your referring dentist, particularly if part of the tooth has been lost to decay, has a large filling or undergone trauma. A crown or other restoration is usually needed to further protect and restore the tooth to full function and is extremely important in ensuring long-term success. Contact your referring dentist as soon as possible to arrange for any necessary treatment.
