Clinical Science
Campbell Clinic Foundation: Research Partner and Pioneer
Campbell Clinic and Campbell Clinic Foundation are partners in conducting orthopaedic research studies with the goal of improving patient care and advancing knowledge. We work with dozens of leading healthcare and scientific institutions around the world in all orthopaedic subspecialties. Our impact is felt at home and around the world.
Currently, we facilitate more than 140 active research studies ranging from retrospective record review to randomized clinical trials. Campbell Clinic is a valued partner in industry-funded, collaborative and study group research studies.
We track productivity by evaluating our clinicians, fellows and residents contributions to peer-reviewed publications and presentations at medical society meetings. With the exceptional leadership of the Campbell Foundation Research Committee (CFRC), study volume and depth continue to expand year over year.
Achievements and Awards
Congratulations to our Campbell Clinic Investigators for their recent recognition in their respective sub-specialty fields:
Pediatric Orthopaedic Society of North America, Best Clinical Science Research Paper
Winner, 2024
David D. Spence, MD and the FACTS (Function After Adolescent Clavicle Trauma and Surgery)
Study Group, Outcomes Following Operative vs. Nonoperative Treatment of Completely Displaced MidShaft
Clavicle Fractures in Adolescent Baseball Player and Other Overhead Athletes
American Shoulder and Elbow Surgeons, Charles S. Neer Award, 2023
Thomas W. Throckmorton, MD, William P. Polio, MD, Blake Hajek, MD, Tyler J. Brolin,
MD, William M. Mihalko, MD, PhD, Kunat Singhal, PT, PhD, Shannon Hughes PT, DPT, EdD,
OCS, MCT, Alexis Nelson Tranum, Tristan Hayes, MSc, Chi-Yang Chiu, PhD, David L. Bernholt,
MD, Frederick M. Azar, MD Muscle Activation Patterns during Active External Rotation
after Reverse Total Shoulder Arthroplasty: An Electrophysicological Study of the Teres
Minor and Associated Musculature
American Association Hip and Knee Surgeons Clinical Research Award, 2023
Mateo J. Kirwan, MD, Zachary R. Diltz, MD, Derek T. Dixon, BS, Carlos A Rivera-Peraza,
BS, William M. Mihalko, MD, PhD, James W. Harkess, MD, James L. Guyton, MD, John R.
Crockarell, MD, Marcus C. Ford Postoperative Oral Tranexamic Acid in Total Knee Arthroplasty: A Randomized Controlled
Trial
Campbell Orthopaedic Journal
The Campbell Orthopaedic Journal is once-yearly publication produced by the Campbell
Clinic Foundation. It features the newest research articles by our graduating class
of resident physician and highlights the Campbell Residency program as well as staff
and resident research efforts from the previous year.
Campbell Clinic and Campbell Foundation work with domestic and international research partners.
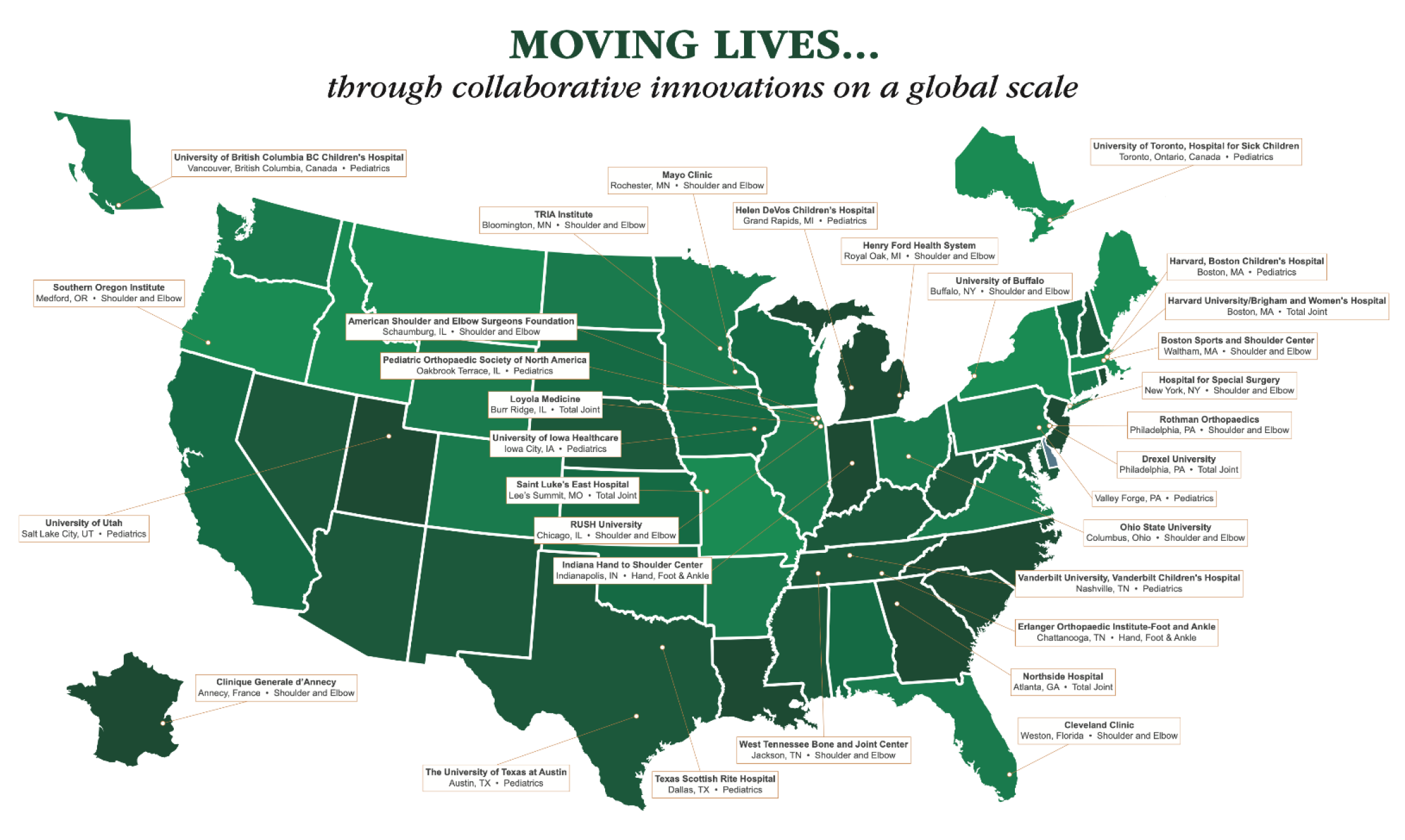
Research partners are in alphabetical order:
- American Shoulder and Elbow Surgeons Foundation
Schaumburg, IL - Shoulder and Elbow - Boston Sports and Shoulder Center
Waltham, MA - Shoulder and Elbow - Cleveland Clinic
Weston, FL - Shoulder and Elbow - Clinique Generale d'Annecy
Annecy, France - Shoulder and Elbow - Drexel University
Philadelphia, PA - Total Joint - Erlanger Orthopaedic Institute-Foot and Ankle
Chattanooga, TN - Hand, Foot, and Ankle - Harvard, Boston Children’s Hospital
Boston, MA - Pediatrics - Harvard University / Brigham and Women’s Hospital
Boston, MA - Total Joint - Helen DeVos Children’s Hospital
Grand Rapids, MI - Pediatrics - Henry Ford Health System
Royal Oak, MI - Shoulder and Elbow - Hospital for Special Surgery
New York, NY - Shoulder and Elbow - Indiana Hand to Shoulder Center
Indianapolis, IN - Hand, Foot, and Ankle - Loyola Medicine
Burr Ridge, IL - Total Joint - Mayo Clinic
Rochester, MN - Shoulder and Elbow - Northside Hospital
Atlanta, GA - Total Joint - Ohio State University
Columbus, OH - Shoulder and Elbow - Pediatric Orthopaedic Society of North America
Oakbrook Terrace, IL - Pediatrics - Rothman Orthopaedics
Philadelphia, PA - Shoulder and Elbow - RUSH University
Chicago, IL - Shoulder and Elbow - Saint Luke's East Hospital
Lee’s Summit, MO - Total Joint - Southern Oregon Institute
Medford, OR - Shoulder and Elbow - Texas Scottish Rite Hospital
Dallas, TX - Pediatrics - TRIA Institute
Bloomington, MN - Shoulder and Elbow - University of British Columbia, BC Children's Hospital
Vancouver, British Columbia, Canada - Pediatrics - University of Buffalo
Buffalo, NY - Shoulder and Elbow - University of Iowa Healthcare
Iowa City, IA - Pediatrics - The University of Texas at Austin
Austin, TX - Pediatrics - University of Toronto, Hospital for Sick Children
Toronto, Ontario, Canada - Pediatrics - University of Utah
Salt Lake City, UT - Pediatrics - Valley Forge, PA - Pediatrics
- Vanderbilt University, Vanderbilt Children’s Hospital
Nashville, TN - Pediatrics - West Tennessee Bone and Joint Center
Jackson, TN - Shoulder and Elbow
